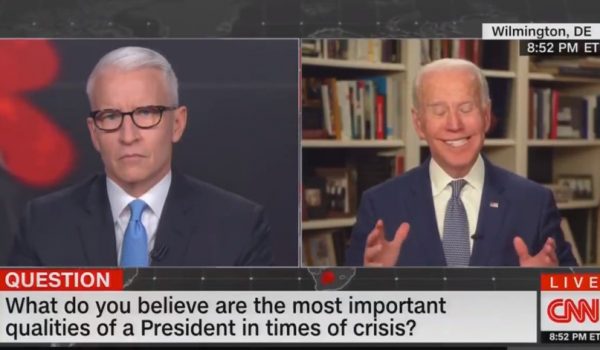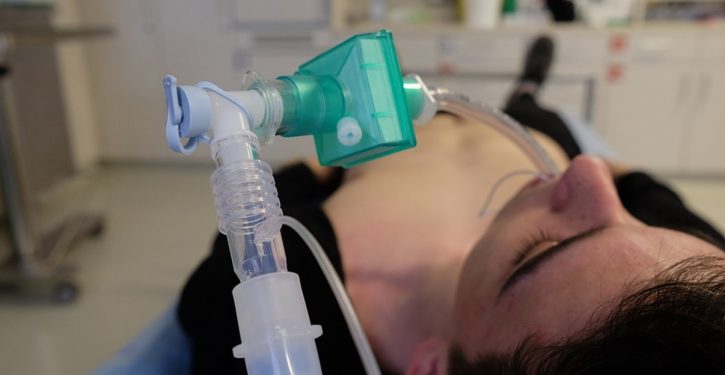
A New York Times article on 29 March 2020 outlines some of the saga of an unsuccessful attempt by the U.S. Department of Health and Human Services (HHS) to get a new-generation portable ventilator developed and procured, for inclusion in America’s Strategic National Stockpile.
The key words in that sentence are “some of.”
The short version of the story is simple. The need for such a project was outlined in 2007. A $6.7 million contract for research and development (R&D) on the desired ventilator – which was to cost the government less than $3,000 a copy – was awarded in 2010. (The original bid solicitation is here.)
The ventilator was duly developed and approved by the FDA; on schedule, we might add.
No ventilators were purchased by HHS. The original contract didn’t include a purchase agreement. A purchase decision was to come later, contingent on federal government resources (p. 21 of the “preparedness strategy” implementation plan shows this in chart form; see “Ventilators” row and footnote 30 on “Programmed procurements” column. The cell entry, “DSNS,” refers to the Strategic National Stockpile. See the bottom of p. 72 for a general statement of the requirement as an element of strategy implementation).
In 2014, a new contract was awarded to a different company to develop a next-generation portable ventilator. This contract was made with the explicit option of ordering 10,000 copies of the ventilator once it was approved. The ventilator was approved in 2019. There are now 10,000 ventilators on order (see NYT article).
What happened to the first contract? The NYT story implies that a big company, Covidien, which had bought out the small original contractor, Newport Medical Instruments, in 2012, decided it (Covidien) didn’t want to go with the Newport product because Covidien owned other ventilator makers. The basic idea is that Covidien bought out Newport to suppress the competition.
Covidien didn’t tell NYT that. This commentary is based on speculation by a third-party industry watcher consulted by the NYT.
We may note, however, that Medtronic, which subsequently bought out Covidien, is still marketing Newport-branded ventilators, one of which, the portable Newport HT70, is substantially similar to the product Newport developed for the contract with HHS.
We know it’s substantially similar because the FDA said it was (scroll down), when it awarded pre-market approval to the HHS-contract product (called the Newport AURA, in honor of the HHS project designation, “Project Aura”). The FDA approval was given in November of 2012. Indeed, federal officials touted it in reports to Congress as a success for their strategic planning effort and their ventilator project.
The Newport HT70, meanwhile – the substantially similar industry product – had received FDA approval in 2011.

This arresting point raises the question why exactly it was necessary to have HHS’s Biomedical Advanced Research and Development Authority (BARDA) contract in 2010 to develop a ventilator that Newport clearly was already making, considering that the company got FDA approval for it in 2011.
The timeliness of what Newport was doing in 2010-2011 can be put down to the significance for industry of hearing signals from the customer. When HHS said in 2007 that a new generation of portable ventilators was needed, the medical device industry would have taken notice.
And HHS wouldn’t have been the only customer sending that signal (indeed, in 2007, HHS was actually listening to the industry itself in making that assessment, as testified to the House of Representatives in 2012 by HHS’s then-Deputy Assistant Secretary for Preparedness and Response, Edward J. Gabriel; link above). Hospitals, doctors, emergency services (a major sector of the portable ventilator market), and medtech marketers would have been sending the signal about ventilators as well.
It’s no mystery why Newport would have been working on or producing a next-gen ventilator. It does require explanation why the federal government trundled along from 2007 to 2010 under the apparently unchanged assumption that the ventilator it sought still required $6.7 million’s worth of developing. (To the answer “That’s the way things are done,” the response is: “That’s my point. We may not being doing things the right way.”)

Note, by the way, that Newport’s HT70 appears to go for about $8,000-9,000 apiece today, depending on features. But as the NYT story indicates, Newport was basically prepared to sell the substantially similar AURA to HHS in bulk for considerably less than that; i.e., at “below $3,000” each. The order never came to fruition.
At any rate, that’s just one aspect of the “rest of the story.”
The “O” word
The most significant aspect is one that isn’t even hinted at in the NYT article. NYT attributes the melancholy termination in 2014 of the languishing 2010 contract – ultimately owned by Covidien – to the Newport buy-out; to a mad dash for such mergers in the timeframe (the mid-2010s); and to Covidien’s decision not to go forward with a sale based on the Project Aura product. To save time, I’ll convey the overall impression in blunt terms: bad, profiteering industry! Bad!
But why was there a mad dash for medtech industry mergers in the mid-2010s? And why might a medtech company have been reluctant, by 2014, to slice its profit margin down as far as necessary to enthusiastically take a low-price, bulk order from the federal government?
Alert readers will have already guessed the main reason, just looking at the dates.
Obamacare, of course.
Obamacare did two things that were frequently – even incessantly – predicted before its provisions began taking effect. It caused a massive scramble for mergers throughout the entire healthcare industry. The increasing load of costly mandates meant that many small actors in the industry simply wouldn’t survive on their own. Fixing that survival problem only increased its urgency; in the case of medical device makers, the bigger and more market-powerful their customers became, the bigger the device makers had to be to survive.
And Obamacare’s specific imposition of a 2.3% medical device tax served to dramatically discourage precisely the things the HHS ventilator project was dealing in: R&D, and bulk, low-margin sales, as the means to build up the Strategic National Stockpile.
As it happened, the 2.3% medical device tax was in effect for only the years 2013-2015. Congress suspended the tax in two-year increments thereafter (and in December 2019 repealed it altogether).
But those two years (and the period of anticipation preceding them) were critical as a catalyst for mergers. And it was right in the middle of them that Covidien would have faced any decision about bulk, low-price sales to HHS. We don’t actually know the particulars of such a decision point for the Newport ventilators. The NYT article doesn’t clarify them (e.g., as to whether there was ever an articulated procurement offer from HHS), and there is no record elsewhere of a procurement offer.
Like everyone else in the medical device industry, Covidien would have confronted a huge increase in its federal tax bill during the years when the device tax was in effect. The tax applied to gross receipts, not to after-cost profits. Some industry executives testified to Congress that the device tax had increased their total federal tax bills by as much as 29%. Because it applied to gross receipts, there was no gain from distributing the device tax’s cost across products of differing profitability. Every dollar of sales, regardless of the profit it represented, was taxed at 2.3%.
So it’s quite possible that selling the Newport AURA to HHS – for, say, $2,995 each – would have cost Covidien money, once the device tax was paid.
We don’t know, because it apparently didn’t occur to the NYT authors to ask. We do know that the new R&D contract awarded in 2014 – to a different company, Philips Respironics – was for $13.8 million up-front for the R&D, with a fixed-price option for HHS to purchase 10,000 of the resulting ventilators for $32,800,000. (I.e., $3,280 apiece.)
The purchase now being made for the national stockpile is being made without the costly imposition of the since-repealed medical device tax. That, plus the increase in the projected purchase price for the federal stockpile (i.e., from “below $3,000” to $3,280 apiece), much improved the likelihood of the ventilator project actually resulting in a sales agreement.
That’s some of the rest of the story. It seems to shed some useful light on why things turned out as they did. We may still want to answer the question why we need taxpayer-funded R&D efforts that lag what private industry is already doing, but that’s a question for another day.